The Future of Robotic Surgery
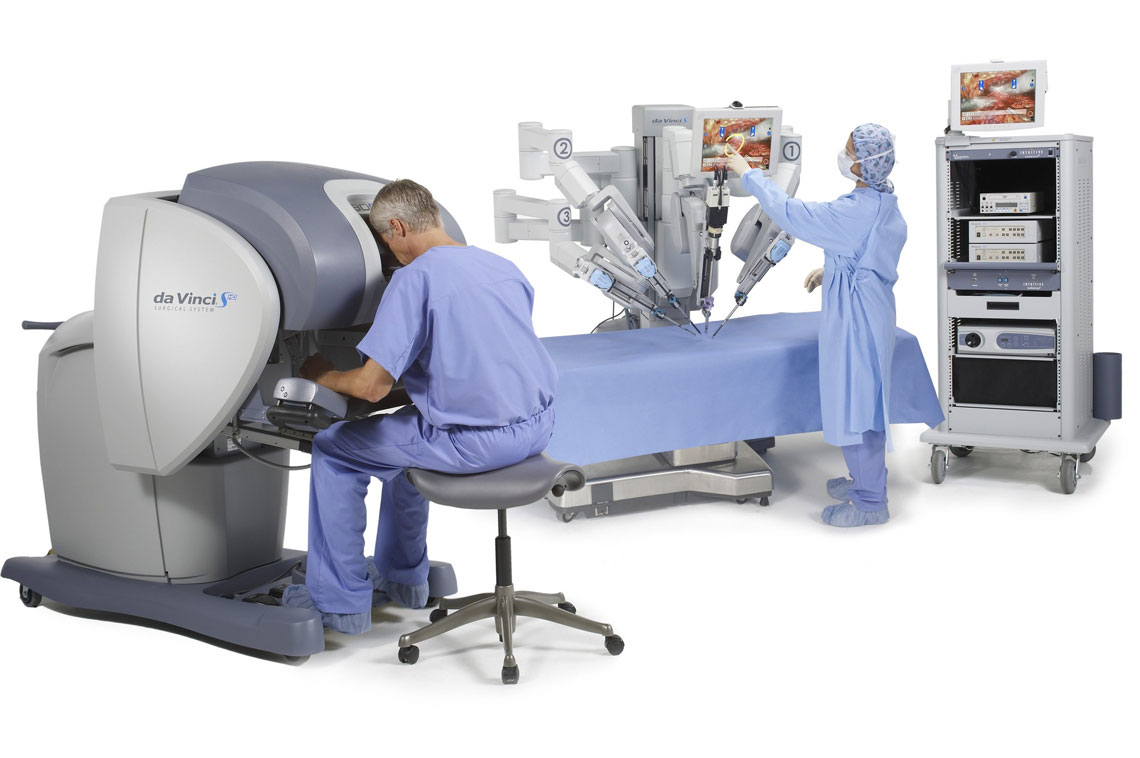
The Future of Robotic Surgery
Many of current advantages in robotic assisted surgery ensure its continued development and expansion. For example, the sophistication of the controls and the multiple degrees of freedom afforded by the Zeus and da Vinci systems allow increased mobility and no tremor without comprising the visual field to make micro anastomosis possible.
Many have made the observation that robotic systems are information systems and as such they have the ability to interface and integrate many of the technologies being developed for and currently used in the operating room. One exciting possibility is expanding the use of preoperative (computed tomography or magnetic resonance) and intra-operative video image fusion to better guide the surgeon in dissection and identifying pathology. These data may also be used to rehearse complex procedures before they are undertaken. The nature of robotic systems also makes the possibility of long-distance intra-operative consultation or guidance possible and it may provide new opportunities for teaching and assessment of new surgeons through mentoring and simulation.
Much like the robots in popular culture, the future of robotics in surgery is limited only by imagination. Many future “advancements” are already being researched. Some laboratories, including the authors’ laboratory, are currently working on systems to relay touch sensation from robotic instruments back to the surgeon. Other laboratories are working on improving current methods anrobot3d developing new devices for suture-less anastomosis.The possibility of automating some tasks is both exciting and controversial. Future systems might include the ability for a surgeon to program the surgery and merely supervise as the robot performs most of the tasks. The possibilities for improvement and advancement are only limited by imagination and cost.
For Intuitive Surgical, microsurgery is a target for research, but not a confirmed direction for development. But a microsurgical robot built by researchers at the Eindhoven University of Technology in the Netherlands is currently in clinical trials, with results expected by 2015. The unnamed bot is operated with dual joysticks and a foot pedal that adjusts the scale.
It’s initially intended for complex reconstructive procedures in the hand and face, offering increased precision for microscopic procedures, such as connecting nerve fibers and tiny blood vessels.
The NeuroArm, a robot that can perform micro-scale neurosurgery while a patient is undergoing an MRI, has already been used in Canada to remove a 21-year-old patient’s brain tumor. The bot, which uses non-ferrous materials (to avoid interacting with the MRI’s magnets), was acquired by surgical imaging firm IMRIS, and has since been rebranded as the SYMBIS Surgical System. SYMBIS isn’t available for sale yet, but IMRIS already sells specialized MRI systems, which allow for scans mid-procedure. Once it’s cleared for use, SYMBIS would allow the surgeon to image the patient’s brain without removing instruments.
There are other examples of microsurgical bots currently in development, including Johns Hopkins University’s Steady-Hand Eye Robot, which deals solely with retinal procedures, and Carnegie Mellon University’s Micron, a handheld robotic instrument that would use gyroscopes and actuators to actively boost the precision of the surgeon. All of these systems are years and possibly decades from use, if they make it to market at all. But Intuitive Surgical interest in microsurgery is a clear indication of what’s to come. Despite a series of lawsuits leveled at the company in 2013, and the subsequent negative media coverage and pummeling in the stock market, Intuitive is the biggest maker of surgical robots, and one of the driving forces in the entire robotics industry, with systems that routinely sell for more than $2M, and more than 200,000 da Vinci procedures conducted yearly. And according to Mohr, adding micro-scale capabilities might not require entirely new robots, but rather new instruments and other modular components that would attach to some portion of the more than 2500 da Vinci’s already installed worldwide.
For us prospective patients, it doesn’t necessarily matter who makes microsurgery more accessible. What matters is that it’s coming.
“We as a medical community haven’t made a lot of therapies that require that kind of super microscopic view and manipulation, because those are at the limit of what the human hands can do at unscaled motion,” says Mohr. “But if we kind of break that barrier, I think it will unleash a lot of new therapies that will have profound effects on patients’ lives.”
Many general surgeons are adding robotics to their scope of practice, but most are taking a wait-and-see approach for several reasons. For some surgeons, the technology is simply inaccessible. Others think the currently unfavorable cost/benefit equation makes the expense of adding robotics wasteful, if not ridiculous.
But many physicians are watchfully waiting, seeking more clarity in the face of current uncertainty. It is no wonder that questions and concerns remain: Will robotics enhance the ability of general surgeons to broaden their scope of practice, make the practice of surgery more fulfilling, and add value to the services provided? To address these questions and to assist general surgeons in making decisions about the value of robotic technology for themselves and their patients, this article offers some perspective on what the future may hold. The speculations presented here are based on personal experience and the history of robotic surgery to date. In addition, this article addresses the pathway for safely introducing robotics into practice as it applies to both practicing surgeons and residents in training.







